Matt Pratt-Hyatt
Chief Science Officer, KBMO
In this blog we delve into the important communities that are living within us; more specifically I am referring to fungal and bacterial microbials.
About 100 trillion microbes inhabit the human gut, and they also inhabit other parts of the body such as the throat, upper respiratory tract, and skin (1). As the large number of cells associated with these microbes and their metabolites are absorbed into the blood stream, it is important to make sure that their population is managed correctly.
Overabundance of pathogenic microbes can cause many different conditions, including problems with mood, cognition, energy, immune systems, and inflammation (Figure 1) (2). Within the Metabolic Insights Profile (MIP) Test, we have put together the most diverse selection of markers to cover a vast spectrum of different microbial pathogens.
Fungal Microbials
Our first group of markers within the MIP help to diagnose overgrowth of different types of fungal microbials. Fungal pathogens cause more than a billion human infections and at least 1.6 million deaths per year (3).
There are many different types of fungal species, and the markers for them can differ. Our first three markers are broad-spectrum fungal markers to help identify overgrowth. The first two are arabinose and arabitol. Different fungal species produce arabitol in the body which is then converted to arabinose; though it should be noted that arabinose can also be present in the urine from dietary sources (4). A third generic fungal marker is citramalic, produced from multiple species of yeast. High values of any of these three markers can indicate a fungal overgrowth (5). Utilizing this trio combination gives the most accurate assessment of a possible fungal overgrowth.
Pathogenic Mold
Besides identifying general overgrowth, we are very interested in detecting colonizations of many different species of pathogenic mold. Some of the more common types of molds that can colonize humans are aspergillus, fusarium, and penicillium (6, 7). These molds can release toxins (known as mycotoxins), which can lead to a whole host of different health problems for the patient. About a third of patients with elevated mycotoxins have overgrowths of these different mold species (8). By utilizing three different markers that are specific for mold colonization, we can help to individualize care for many different types of ailments.
Bacterial Overgrowths
More common than fungal overgrowths are bacterial overgrowths. Overgrowths of bacteria in the intestines, or overabundance of pathogenic bacteria can lead to many different types of diseases.
The toxins that pathogenic bacteria produce are associated with many different physiological issues, including inflammation, lower nutrient absorption, inhibition of neurotransmitter metabolism and many more (9). One of these toxins is a marker called HPHPA, which is produced by Clostridia. This marker, which is found in higher amounts in adults with recurrent diarrhea, is a metabolite of m-tyrosine. HPHPA inhibits the enzyme dopamine-beta-hydroxylase (10, 11), which can lead to imbalance of neurotransmitters, leading to anxiety and symptoms of Obsessive Compulsive Disorder (OCD).
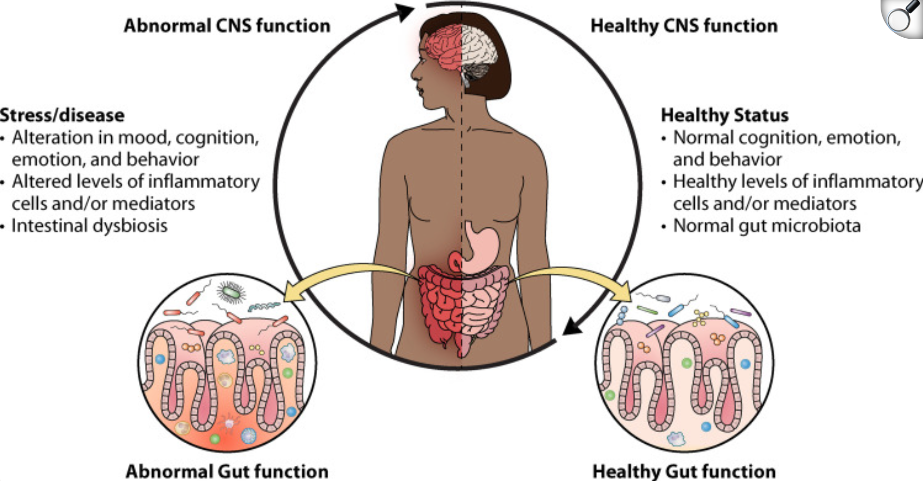
(Figure 1) (2)
By utilizing markers 9-12 on the MIP, practitioners can get an insight into whether their patient is suffering from the effects of pathogenic bacteria. These bacteria could be the cause of the patient’s ailments, or a comorbidity caused by an impaired immune system due to other ailments.
Within the MIP we also have other, more broad-spectrum bacterial markers that can help identify a bacterial overgrowth. These markers are numbered 13-18. Most elevations in these markers are signs of dysbiosis and should be treated accordingly.
Want to Learn More?
If you’re interested in learning more about how organic acids can provide insights into fungal and bacterial pathogens in your patients, please contact us here.
The KBMO Diagnostics Metabolics Insights Profile (MIP) provides a full metabolic snapshot for your patients, including markers that can reveal issues such as nutritional deficiencies, microbial overgrowth, toxic exposure, oxalates, mitochondrial impairment, neurotransmitter imbalances and much more.
References:
- R. Tojo et al., Intestinal microbiota in health and disease: role of bifidobacteria in gut homeostasis. World J Gastroenterol 20, 15163-15176 (2014).
- S. G. Sorboni, H. S. Moghaddam, R. Jafarzadeh-Esfehani, S. Soleimanpour, A Comprehensive Review on the Role of the Gut Microbiome in Human Neurological Disorders. Clin Microbiol Rev 35, e0033820 (2022).
- A. Rokas, Evolution of the human pathogenic lifestyle in fungi. Nat Microbiol 7, 607-619 (2022).
- J. Nekvapil, D. Sumczynski, R. N. Salek, M. Buckova, The Release of Organic Acids and Low Molecular Weight Carbohydrates from Matcha Tea After In Vitro Digestion. Nutrients 16 (2024).
- M. Amaha, T. Sai, Some aspects of (-)-citramalic acid accumulation by respiration-deficient mutants of yeasts. Antonie Van Leeuwenhoek 35, Suppl:G15-16 (1969).
- E. M. Rick, K. Woolnough, C. H. Pashley, A. J. Wardlaw, Allergic Fungal Airway Disease. J Investig Allergol Clin Immunol 26, 344-354 (2016).
- L. T. Roland et al., Diagnosis, Prognosticators, and Management of Acute Invasive Fungal Rhinosinusitis: Multidisciplinary Consensus Statement and Evidence-Based Review with Recommendations. Int Forum Allergy Rhinol 13, 1615-1714 (2023).
- M. Pratt-Hyatt, Biochemical Markers in the Urine Associated with Gastrointestinal Mold-Overgrowth Are Linked with Elevated Urinary Mycotoxins in Patients with Suspected Mold Illness. Townsend Letter 31 (2019).
- R. Chandrasekaran, D. B. Lacy, The role of toxins in Clostridium difficile infection. FEMS Microbiol Rev 41, 723-750 (2017).
- X. Xiong, D. Liu, Y. Wang, T. Zeng, Y. Peng, Urinary 3-(3-Hydroxyphenyl)-3-hydroxypropionic Acid, 3-Hydroxyphenylacetic Acid, and 3-Hydroxyhippuric Acid Are Elevated in Children with Autism Spectrum Disorders. Biomed Res Int 2016, 9485412 (2016).
- W. Shaw, Increased urinary excretion of a 3-(3-hydroxyphenyl)-3-hydroxypropionic acid (HPHPA), an abnormal phenylalanine metabolite of Clostridia spp. in the gastrointestinal tract, in urine samples from patients with autism and schizophrenia. Nutr Neurosci 13, 135-143 (2010).